Abstract
Nursing, as a progressive and developing profession, requires those who engage in it to demonstrate well developed critical thinking, as early as their undergraduate training. Reflection skills are a mechanism for developing critical thinking and they form part of the core of the nursing training programme. Preceptors have a major role in helping students perform reflection, through guided reflection that facilitates the development of critical thinking. Nonetheless, it is hard to instil productive reflective thinking in students and to sufficiently develop their critical thinking. An academic nursing school in central Israel developed a tool called Reflective Nursing Debriefing (RND), based on well-established principles of reflection, which constitutes an initiated, systematic and structured reflective learning tool for the development of critical thinking. This tool is used by students to perform reflection and by preceptors for the purpose of monitored involvement in guided reflection. In practice, preceptors do not achieve full utilization of the tool, and thus students are not exposed to its potential contribution to developing their critical thinking. The case study presented in this paper portrays the issue by analysing three cases that utilized this tool, with the preceptor employing guided reflection, and it suggests important recommendations for preceptors. Additionally, it offers professional nursing education recommendations with regard to the system's responsibility for achieving professionalization of preceptors. This will help preceptors use the tool properly and develop a prominent skill necessary for guided reflection and in general, develop better critical thinking among students.
Keywords: Preceptor rolereflectionguided reflectionnursingcritical thinking
Introduction
Nursing practice is at present very different from the past, and it is continuing to evolve as the 21st century progresses (Berman, Snyer & Frandsen, 2016). In the changing global society, the role of nursing has been transformed from a traditional role focusing on the provision of medical aid to people centred care that requires the nursing practitioner to demonstrate high autonomy and responsibility (Tashiro et al., 2013). Nursing students who complete their studies in a professional training programme begin work in the profession as novices. As novices, they have at their disposal the skills they acquired through theoretical studies and particularly through clinical studies provided in the various clinical domains as part of their professional training. These novices are considered nurses inexperienced in the various situations they encounter in their nursing practice. They perform basic skills and operations in response to the client's problems. Their ability to employ professional discretion and judgment is rudimentary. They are indeed guided and directed in performing their role by procedures and directives, but these procedures cannot guide them in making decisions and applying the correct skills in an actual unanticipated situation (Marble, 2009; Benner, 2001). In order to produce novice nurses who display more advanced, independent and responsible professional discretion and judgment upon entering the profession, the professional training programme must make greater efforts to develop the critical thinking of nursing students.
Critical thinking is a process that involves seeking, receiving, evaluating, analysing, integrating and conceptualizing information, with the purpose of developing conscious thinking and the capacity to utilize the information creatively and to take risks. It is a fundamental way of thinking in order to solve problems and reach clinical decisions in daily nursing practice (Yildirim & Ozkahraman, 2011). Throughout the years critical thinking in nursing has been receiving growing attention, however the efficacy of educational interventions aimed at developing and improving this type of thinking remains unknown. Educational interventions constructed with the purpose of improving the ability to apply discretion and to make decisions are complex and studies have shown that there is no certified method for teaching the subject and for training learners (Thompson & Sally, 2011). Nonetheless, self efficacy, self confidence, organizational capacity, nursing education and support were found to be significant factors that influence effective clinical decision making (Hagbaghery, Salsali & Ahmadi, 2004). One of the skills that facilitate these factors in the learning process is that of reflection. The next section will discuss the skill of reflection in the context of developing critical thinking as well as with regard to the educational figure that may help develop critical thinking through use of this skill.
Reflection and critical thinking
Reflection is defined as "a process of reviewing an experience of practice in order to describe, analyze, evaluate and so inform learning about practice" (Reid, 1993: 305). Much has been written about the skill of reflection in the context of learning processes in professional practice. This skill is a vital and integral part of developing the decision making process in the nursing profession (Truglio-Londrigan & Lewenson, 2008) and therefore it is taught in nursing training programmes (Braine, 2009). The purpose of reflection is to bring the internal process that takes part within one's self to a state of open professional discourse, to lend learning a methodical and well-shaped design, and to improve professional behaviour. This process involves a situation or an endeavour that triggers questions, leading to further exposure and learning (Conte, 2015). In this way, the role of reflection is to create a high standard process of professional thinking and learning (Conte, 2015) as well as logic-based practice (Bulman, Lathlean & Gobi, 2012).
Reflection can take place before, during, or after an incident (Rogers, 2001). The type of reflection that is commonly used as an exercise in decision making processes for students in the various healthcare professions is reflection on action (Conte, 2015; Wainwright, Shepard, Harman & Stephens, 2010). Reflection on action is the retrospective analysis of a behaviour that occurred previously, with an emphasis on self-questioning and feedback from others (Rogers, 2001). The essential skills for reflection are self awareness, description, critical analysis, synthesis and evaluation (Atkins & Murphy, 1993). These reflection skills are a mechanism for developing critical thinking and they are utilized in the training programme, however it remains difficult to instil in students efficient reflective thinking as well as to develop their critical thinking on the anticipated level. Students often lack the ability to perform reflection and are consequently only capable of describing the situation (Conte, 2015). The person capable of guiding students in thorough reflective thinking and helping them develop critical thinking is the preceptor.
The role of the preceptor in the student's assimilation of the reflective process
Preceptors constitute the main link in the curricular transition from theoretical knowledge to clinical practice in the field. Their role is to promote critical thinking and problem-solving skills that form the essence of an academic education (Carlson, Wann-Hansson & Pilhammar, 2009). They are also expected to direct students towards organizing their behaviours and strategies for achieving effective and efficient patient care (Barker & Pittman, 2010). For this reason, it is important that preceptors find the time to support students in reflecting on their clinical practice, for which one of the tools at their disposal is guided reflection (Duffy, 2009). Guided reflection is a supportive collaborative process, a journey from one's present place to where one wishes to be (Johns, 2002). Active involvement of preceptors in the reflection processes of students through guided reflection is valuable for the learning process (Conte, 2015). Preceptors are in an ideal position to undertake this responsibility (Duffy, 2009), since clinical studies in the field create genuine opportunities for reflection on real scenarios (Conte, 2015). Preceptors can help students who encounter difficulties with interpreting incidents in which they were involved in the field in order to achieve continuous clinical learning needs (Duffy, 2009) in real time.
The ability to ask challenging and thought provoking questions may be the most valuable skill that the preceptor can offer for guided reflection of the student's reflective process. Suitable questioning may stimulate critical thinking by the student and improve the student's problem-solving and decision-making skills (Duffy, 2009). The goal is for students to be able to ask themselves similar questions to those asked by the preceptor (Dekker-Groen, Schaaf & Stokking, 2012), as professionals are expected to be responsible for their learning throughout their professional life (Conte, 2015). This in order to be safe, caring, and professionally competent nurses. A structured tool called Reflective Nursing Debriefing was developed in order to help students with the reflective process and preceptors with guided reflection.
Learning tool: Reflective Nursing Debriefing
As part of a study training programme in nursing, an academic nursing school in central Israel developed a reflective tool called Reflective Nursing Debriefing (RND). This tool was constructed based on features of reflection described in the literature. The RND tool is an initiated, consistent, systematic reflective-retrospective learning tool (reflection on action) for understanding professional operations, interpreting the meaning of successes and lapses, reaching conclusions and learning lessons, formulating insights, and assimilating and applying them in future activities of students as individuals. These components are similarly described in the literature as features of good reflection: association with past, present and future experiences, integration between cognitive and emotional experiences, referring to an incident from multiple aspects, declaring lessons learned, planning future conduct in a similar incident (Aronson, 2011) and providing feedback.
When using the RND tool (Figure
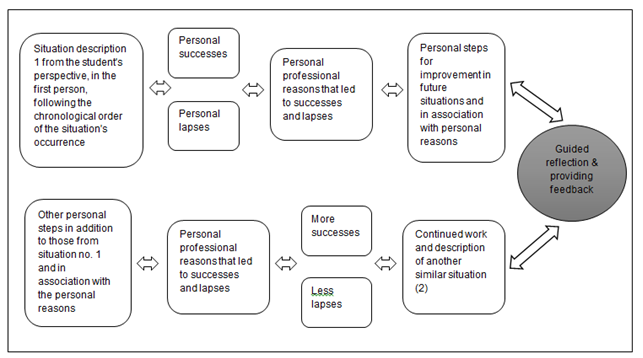

Problem Statement
This tool was used at the school at which it was developed by some 120 preceptors in in-patient and community-based clinical fields, as well as by 400 students, during 2013-2017. Despite its declared goals, preceptors have not been maximizing the tool's abilities with regard to critical thinking and have not been making optimal use of guided reflection. This is evident from the reports of students and preceptors on use of the tool and from inspection of the tool products submitted to the school as part of the requirements for clinical studies. Some students perceive reflection as extra work, since they do not understand how reflection affects their learning or are not motivated to use it (Conte, 2015). Thus, to a certain degree students perceive the RND tool merely as a type of chore, since when presenting reflection findings the study discourse between preceptor and student through guided reflection amounts in practice to mere discussion of the procedures (laws and structural directives). It does not include development of advanced independent clinical thinking and wide professional responsibility.
To demonstrate this, the current paper shall present an analysis of three cases in which the tool was used for guided reflection with the preceptor's involvement.
Research Questions
What is the student's potential of learning from the guided reflection process facilitated by the RND tool?
Purpose of the Study
To examine the student's potential of learning from the guided reflection process facilitated by the RND tool.
Research Methods
Research Strategy
This study used a case study strategy in order to analyze the student's reflection based on the RND tool.
Research Population
The research population consists of three Israeli nursing students at an academic school of nursing in central Israel, studying in different tracks and at different stages of their studies.
Sampling Method
The sampling method selected for this study is the purposive sampling method that focuses on selecting participants most representative of the phenomenon studied.
Findings
Analysis of the three cases indicated the student's potential of learning from the guided reflection process facilitated by the RND tool, as follows:
Case 1: Potential of learning from success beyond a written set of rules
A student at an advanced stage of his clinical studies described a situation in which he realized that a patient under his care who was anesthetized and on artificial respiration was not wearing a medical ID bracelet stating the patient's sensitivities, as required by department procedures. This patient was sensitive to sulpha. The student described the situation using the RND tool and wrote that he noticed the absence of a suitable bracelet, reported this to the preceptor, and a sensitivity bracelet was added to the current one. The student said: "I made sure to follow the procedures and I identified the lapse" and stated that prior to any treatment of a patient it is necessary to identify the patient and to check sensitivities. The preceptor provided positive feedback on the student's analysis of the situation. The student felt good about his management of the incident and the process of learning through the tool appeared to have fulfilled its goals. However, the student indeed identified the lapse involving the lack of an appropriate medical ID bracelet, but this is not sufficient considering the stage he had reached in his studies. The student analysed the case only on the procedural level, and performed basic analysis. i.e., analysis following a written set of rules. Questions the preceptor could ask for more advanced analysis are: Who should be informed of the incident aside from the preceptor? For what reason? Through these questions it would have been possible to bring the student to think about his wider responsibility to report the incident. In this case it was necessary to report to the head nurse, as she can assess whether this is an isolated incident or a departmental norm and, accordingly, intervene and improve practice processes. Other questions that could be asked are: What could have happened if you had not realized that the patient was missing an appropriate bracelet, or what implications could the lack of such a medical ID bracelet have? Another question could lead to clarifying what medication had been administered to the patient until the lapse was recognized. Another question: From what stage of the patient's hospitalization do nurses check medical ID bracelets as part of regular practice? This is another possible question concerning clarification of the admission procedure. In other words, these are details to which the student did not attend and he was not aware of all the aspects of his responsibility with regard to the incident or with regard to reporting to other superiors. This constitutes learning beyond a written set of rules.
Case 2: Potential of learning from mistakes as a catalyst for anticipating the unexpected
A student at an initial stage of her clinical studies, who had practiced a simulation involving connecting a patient to an infusion set, described an incident in which she was requested to connect a patient under her care to an infusion set following the medical instructions. After connecting the bag to the set, she rinsed out the infusion system and approached the patient. While the student was repeating the rinse at the sink next to the patient's bed, the tip of the set that is attached to the intravenous catheter touched the sink. The patient noticed this and mentioned it to the student. The next day the student attempted to replace an infusion bag and during the replacement the tip of the infusion set touched her coat. The preceptor following the process stopped the student because she did not notice this herself. The student wrote in the case analysis: "On the first day I held the tube of the infusion set far from the tip and the tip swung and touched the sink. On the second day it happened because I did not plan in advance where to throw away the bag. The necessary step for improvement in the future is that I must think about possible complications in advance at the planning stage. Good planning prevents lapses." In this case as well, the impression is that the student learned an essential lesson from the situation and, moreover, that she appeared to have understood the connection between her actions in the two cases. As the student said: "I would have reached this insight without RND." From the preceptor's perspective, he provided positive feedback on the student's insights. The outcome is that sometimes it is hard to determine whether a certain activity or experience is appropriate for performing meaningful reflection, as some students may find it hard to reflect and might resist the reflection process (Conte, 2015). Thorough re-examination of this case shows that the preceptor did not truly recognize the potential of using the RND tool and went along with the student's hidden insights and resistance. In fact, the preceptor missed the real difficulty experienced by the student and did not recognize in the situation an opportunity for learning and for developing the student's critical thinking.
The student understood that planning the work environment would prevent him from compromising the sterility of the infusion set in the future. But in practice this is not a sufficient insight from two respects. For one thing, what will happen in an unexpected situation when there is no time to plan the work environment? The second aspect has to do with the person who identified the risk; the compromised sterility of the set in each of the incidents. In the first incident it was the patient and not the student, and in the second incident it was the preceptor and not the student. Furthermore, the question is: How can one identify the relevant risk, i.e., compromised sterility? What will help you identify deviations in an unexpected situation? The preceptor missed the student's essential difficulty with developing self-monitoring mechanisms and anticipating the unexpected, i.e., with identifying the risk in these cases, which is part of the student's professional responsibility.
Case 3: Potential of learning from success as a catalyst for reinforcing perceptions of the nurse's professional role
A student retraining for a career in nursing described an incident in the nephrology unit in which he was involved. The student related that he identified the risk of a fall in the case of an 82 year old patient who had completed his dialysis treatment and attempted to stand up at the end of the procedure. The student made sure that the patient was capable of standing independently and that he was walking well, accompanied by his carer. The student emphasized that he experienced only success in this incident and that a possible fall had been prevented. In this case as well, the preceptor provided positive feedback on the student's decision making: "The student identified the risk of a fall and acted properly." Here too the student seems to have operated optimally. Nonetheless, when examining the critical thinking that the student could have developed by using the tool, upon analysing the three cases described, it is evident that a very major part of the tool's essence was not realized.
The student indeed recognized the patient's risk of a fall. The student wrote that, as a step towards future improvement, "I must anticipate that the patient could be unstable after undergoing dialysis, notice how he gets up from the treatment chair, and make sure that he is accompanied." In arriving at this understanding, the preceptor missed a significant opportunity to enhance the student's perception of the profession by analysing the tool's findings. The necessary question that the preceptor should have asked here is how else can a patient's fall be avoided even before getting up from the chair? This is one possible question that could lead the student to think about overall nursing interventions in the context of preventing falls. Moreover, it would have contributed to his perception of the nursing profession; a perception that encompasses the patient's inclusion and instruction within the nurse's role. This at any time, in order to bring the patient to an optimal level of independence according to his situation.
Conclusion
The limitations of this study are that it refers to three specific cases and their special conditions, and therefore the ability to infer from one case to another is problematic (Harvey, 1990). Nevertheless, Harvey notes that the conclusions of a case study can serve as a point of department for more accurate observation and for initiating a debate or a social discussion.
Student's Point of View
From the student's point of view, the essential foundations of the reflection process are cognitive activities such as analysis and explanation (Dekker-Groen, Schaff & Strokking, 2011). In order to help the student with this, the cases described demonstrate that it is important for the preceptor to ask thought provoking questions as part of the guided reflection on the process. Indeed, the literature lists general structured questions for performing reflection that serve as an aid for the preceptor in the guided reflection (Conte, 2015), as does Table
Certain students might object to use of the RND tool, which constitutes a type of post-action reflective analysis. For this reason it is important to perform the questioning non-judgmentally and non-critically, since these students are sometimes engrossed in a moment of truth as a result of their lack of knowledge or incompetence (Conte, 2015). Moreover, it is important to emphasize to students the process of learning from their mistakes through the questions asked, as well as stressing their strengths (Conte, 2015). It is necessary to bring the student to the understanding that this is a learning process that will lead to success. Preceptors must refer in their questions in the guided reflection to successes in the student's work even in cases of grave mistakes. In this way, the RND as a reflective tool can prevent a sensation of failure and transform the student's experience into one involving a sensation of growth and learning.
Preceptors' Point of View
From the preceptors' point of view, they have little experience with using guided reflection as part of the preceptorship process in the clinical field (Duffy, 2009). Hence, many preceptors do not manage to generate future benefits of using guided reflection supported by the reflective learning process of students (Duffy, 2009). This is also true of use of the RND tool by preceptors. Among the vital necessary skills in this context are coaching skills; the ability to ask challenging thought-provoking questions that can lead one in the process of decision making, to assess the student's work collaboratively and to be attentive to the student's objections and needs (Fielden, 2005). These coaching skills are supported by the literature as part of the preceptor's requirements for guided reflection (Dekker-Groen, Schaff & Strokking, 2011). Coaching skills are complex skills currently considered a distinct profession. Thus, it is evident that the preparation of preceptors in the field for guided reflection, as suggested in the literature (Braine, 2009; Dekker-Groen, Schaff & Strokking, 2011), is insufficient. This is also true of the day-long preparation workshop for guided reflection held at the school for preceptors using the RND tool. There is need for a great deal of effort based on practicing this skill in order for it to be instilled in preceptors. This effort includes a process of ongoing guidance involving situations encountered by the preceptor when accompanying the student, encompassing role modelling of coaching skills and of providing feedback and support. Since the preceptors are the major human resource for training students in the field, the faculty of the university and of the nursing school are responsible for guiding the preceptors and supporting them in this area. Proper extensive use of this tool will lead to realizing its full learning potential, help preceptors in their role, and make it possible to develop better professional critical thinking among the students.
References
- Aronson, L. (2011). Twelve tips for teaching reflection at all levels of medical education. Medical Teacher. 33(3). p.200–205.
- Atkins, S. & Murphy, K., (1993). Reflection: a review of the literature. Journal of Advanced Nursing, 18(8), 1188-1192.
- Barker, E.R. & Pittman, O. (2010). Becoming a super preceptor: A practical guide to preceptorship in today’s clinical climate. Journal of the American Academy of Nurse Practitioners, 22, 144-149.
- Benner, P. (2001). From Novice to Expert; Excellence and Power in Clinical Nursing Practice. New Jersey: Prentice Hall Health.
- Berman, A.,Snyder, S. & Frandsen, G.(2016). Kozier & Erb"s Foundamentals of Nursing: Concepts, Process, and Practice. 10th ed. Boston: Pearson.
- Braine, M.E. (2009). Exploring new nurse teachers’ perception and understanding of reflection: An exploratory study. Nurse Education in Practice, 9, 262-270.
- Bulman, C., Lathlean, J. & Gobbi, M. (2012). The concept of reflection in nursing: Qualitative findings on student and teacher perspectives. Nurse Education Today, 32. e8-e13.
- Carlson, E., Wann-Hansson, C. & Pilhammar, E. (2009).Teaching during clinical practice: Strategies and techniques used by preceptors in nursing education. Nurse Education Today, 29(5), 522-526.
- Conte, N. (2015).Preceptors guidance in students’ self-reflection: An invaluable contribution. Currents in Pharmacy Teaching and Learning, 7, 395-404.
- Dekker-Groen A., van der Schaaf, M. & Stokking, K. (2012).Performance standards for teachers supporting nursing students’ reflection skills development. Journal of Nursing Education and Practice, 2(1), 9-19.
- Dekker-Groen, A. van der Schaaf, M. & Stokking, K. (2011). Teacher Competences required for developing reflection skills of nursing students. Journal of Advanced Nursing, 67(7), 1568-1579.
- Duffy, A. (2009). Guiding students through reflective practice - The preceptors' experiences. A qualitative descriptive study. Nurse Education in Practice, 9, 166–175.
- Fielden, S. (2005). Literature Review: Coaching Effectiveness–a Summary. Manchester: NHS Leadership Centre, University of Manchester.
- Hagbaghery, M., Salsali, M. & Ahmadi, F. (2004). The factors facilitating and inhibiting effective clinical decision-making in nursing: A qualitative study. BioMedical Central Nursing, 3(1), 1-11.
- Johns, C.( 2002). Guided Reflection Advancing Practice. Oxford: Blackwell Publishing.
- Harvey, L. (1990). Critical Social Research. London: Unwin Hyman
- Marble, S. G. (2009). Five-Step model of professional excellence. Clinical Journal of Oncology Nursing, 13(3), 310-315.
- Reid, B. (1993). “But we’re doing it already!” Exploring a response to the concept of reflective practice in order to improve its facilitation. Nurse Education Today, 13, 305-309.
- Rogers, R. (2001).Reflection in higher education: a concept analysis. Innovative Higher Education, 26(1), 37-57.
- Tashiro, J., Shimpuku, Y., Naruse, K., Matsutani, M. & Matsutani, M. (2013). Reflection as a Window to Student Development: Insight for Faculty, Preceptors, and Mentors. Japan Journal of Nursing Science, 10, 170-179.
- Thompson, C. & Sally, S. (2011). Do educational interventions improve nurses' clinical decision making and judgement? A systematic review. International Journal of Nursing Studies, 48, 881-893.
- Truglio-Londrigan, M. & lewenson, S.B (2008). Decision-Making for Nurses: Thoughtful Approaches to Practice. London: Jones and Bartlett Pub.
- Wainwright, S.F., Shepard, K.F., Harman, L.B. & Stephens, J. (2010). Novice and experienced physical therapist clinicians: a comparison of how reflection is used to inform the clinical decision-making process. Physical Therapy, 90(1), 75-88.
- Yildirim, B. & Ozkahraman, S. (2011). Critical thinking in nursing process and education. International Journal of Humanities and Social Science, 1(13), 257-262.
Copyright information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
About this article
Publication Date
28 June 2018
Article Doi
eBook ISBN
978-1-80296-040-2
Publisher
Future Academy
Volume
41
Print ISBN (optional)
-
Edition Number
1st Edition
Pages
1-889
Subjects
Teacher, teacher training, teaching skills, teaching techniques, special education, children with special needs
Cite this article as:
Goldman, I., & Cojocaru, S. (2018). Upgrading Learning In Nursing Preceptorship Using A Reflection Tool. In V. Chis, & I. Albulescu (Eds.), Education, Reflection, Development – ERD 2017, vol 41. European Proceedings of Social and Behavioural Sciences (pp. 1-11). Future Academy. https://doi.org/10.15405/epsbs.2018.06.1

