Abstract
Diagnosing an individual as a victim of cancer is an event that requires the support of the individual in the process of dealing and treating the disease. The purpose of this research is to ascertain which of socio-demographic factors of pacients determine the need for psycho-oncological care. In this paper are presented differences in the need for psycho-oncological help of the patients of different age, different marital status, patients with children and without children and with different levels of education. The problem of the research is to identify which categories of patients have more need for psycho-oncological care. A questionnaire is used to determine the need for psycho-oncological care, which includes the desire of patients to get help in order to manage the disease and the data obtained from the interviews were processed in a qualitative manner. The subject of research were 30 patients suffering from cancer at the University Hospital's Oncology Department Skopje-surveyed in October 2010 to May 2011. The results show that patients aged 45-60 years have more need for psycho-oncological care,also those with secondary education, who are married with children and are in the process of therapy. We can conclude that every person needs care and we should create an individual concept for psycho-oncological care. Patients who have lower socio-economic conditions and which are in the period of acceptance of the disease have a greater need for psycho-oncological care.
Keywords: psycho-oncological carecancerageeducation
Introduction
All people know that a day will come when they would die and that is an unchangable fact. But when it comes to the fact if a man could ever be prepared for death, the answer to this question is hard to give, because even in the most difficult situations man is inclined to hope. Getting ill from a disease which is likely to be fatal when you expect this at least, is the most difficult and cope situation to deal with. Living in difficult situations people seek support from their close circle or from professionals, who will help to overcome the difficulties with as little damage as possible. For these reasons as the purpose of this paper we got patients suffering cancer because that disease for most people in the world is disappointing and hard to accept.
The diagnosis of cancer is a drastic event for a man’s life and his family, so the patient and his family should have a great commitment to the management of the event which helps the further journey. After determining the diagnosis, the patient must undergo several therapeutic interventions with different risks such as surgical interventions, chemotherapy and radiation or cell transplantation. All these interventions lead to a change in physical appearance and also the mental and social life of the patient. The disease has a great impact on everyday life, performing professional duties and the socialization of the patient. He is overwhelmed by the situation, a situation which significantly affects his life further. Depressive reactions of the patient, anxiety or helplessness have an impact on any future diagnostic procedure and therapy, have an impact on the welfare of family and profession. Such emotional condition can adversely affect the patient's cooperation with physicians, therapy and have an impact on physical and mental well-being of him. Therefore vital in these cases is the early diagnosis of mental welfare of the patient and early psycho-oncologycal treatment which would prevent psychological damage, chronic damage and improve patients conscience psycho-oncologycal care.
Given the objective of this research as in theoretical and in practical terms, we will consider the importance of psycho-oncologycal care to rate the importance of psychosocial support to patients with cancer of different ages, with different marital status, with and without children and with different levels of education
Psycho-oncology
Psycho-Oncology is dedicated to counselling, care and treatment of people with cancer and their family and social environment. "Psycho-oncology or "Psychosocial Oncology" is the science that deals with experiences, behaviours and social resources of cancers in context with cancerous diseases and their treatment (Tschuschke 2006 p.32)". Psycho-oncology’s task is to investigate and reveal the psychological and social factors, review the diagnosis, treatment, rehabilitation and care of the further course of the cancer disease and interactions (DGK, Deutsche Krebshilfe, AWMF 2014, p.1).
Psycho-oncology aims are to investigate and examine scientifically methodologies and to apply them in prevention, counselling, early cancer detection, diagnosis, treatment, rehabilitation, palliative care and ambulance care. Psycho-oncology deals not only with people directly affected by cancer, but also with their families and their social environment, therefore there is a need for a more professional care. Characteristic of psycho-oncology is interdisciplinary and highly professional cooperation. For psycho-oncologycal care to patients a cooperation of: doctors, psychologists, psychotherapists, social workers, educators, therapists of art, music, nurses, physiotherapists, speech therapists, clerics, monks etc is needed (DGK, Deutsche Krebshilfe, AWMF, 2014. p.4).
Psycho-oncologycal interventions intend to examine psychological problems and social issues in the context of treatment of cancer diseases, assist patients in facing the disease, to support the state of mind and to accompany the patient to the problems in diagnosis, therapy and to improve the state of mind of his, strengthen social and sociological resources to participate and support patients in order that the life quality of patients and their families be maintained and grow. The main task of psycho-oncological care is the orientation of the patient's needs for psycho-social counselling, psycho-oncological diagnostics, treatment and support for coping with the disease and specific psychological and social treatments (DGK, Deutsche Krebshilfe, AWMF, 2014).
Methodology
The main purpose of this paper is the need to establish psycho-oncological care of patients suffering cancer with different demographic characteristics. The objective of the research was to set socio-demographic factors that are important for psycho-oncological care.
The sample selected for the survey was 30 patients suffering from cancer who were treated in the period from October 2010 to May 2011 at the University Clinic of Skopje-Oncology unit.
In this research was used a questionnaire (also used by psycho-oncologists) that includes the patient wishes to improve coping with the disease. Demographic data included age, education level and family status of the subjects. Also in the research are involved subjects with different treatments of the disease as: patients who receive therapy, patients who have had an operational intervention and patients with metastasis.
2.1. Results
Due to the nature of the questionnaire survey results will be presented in a qualitative way. Results of this research will be presented in the form of percentages and graphical representation. At the beginning, the structure of the sample will be presented as the socio-demographic variables like: family status, different stages of the disease, age, educational level. After presenting the descriptive data the need of different categories of subjects for psycho-oncological care will be presented with the percentage.
All patients involved in this research have children (100%) and 90% of them are married. Patients who are in therapy are 83% of the subjects, 63% of subjects were interviewed after an operational intervention. The research did not have any subject newly diagnosed and 26% of the subjects are in progress of therapy after diagnosis of metastases.
Due to the nature of the disease age structure of subjects is not proportionate. Smaller number of subjects was aged 30-45 years old. This category includes 20% of the total number of subjects (6 people). The largest number of subjects was patients aged 45-60 years old. These are 47% of the subjects involved in research (14 people) and 33% of subjects were aged over 60 years old.
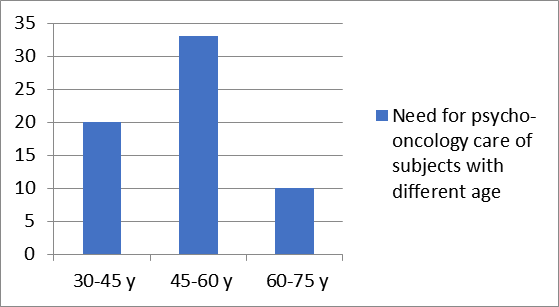
As far as educational status subjects who have not even completed primary education make up 13% of the sample, 18% had completed primary education, 44% are subject who have completed secondary education (general gymnasium), 20% have conducted professional secondary education and 3% of subjects who have completed higher education. In Chart 1 we presented the percentages of subjects of different ages and the need which they represent for psycho-oncological care. 47% of subjects which are aged 45-60 years, 33% of them stated that they have need for psycho-oncological care and 20% of subjects aged 30-45 years and from subjects over 60 years which are 10% express the need for psycho-oncological care. From these results it appears that subjects aged 45-60 years say that they need psycho-oncological care more often than subjects of other ages, but when we analyze the age variable generally 23% of the subjects declare that they need psycho-oncologal care, which makes us think of other factors which encourage cancer suffering patients require psycho-oncological care.
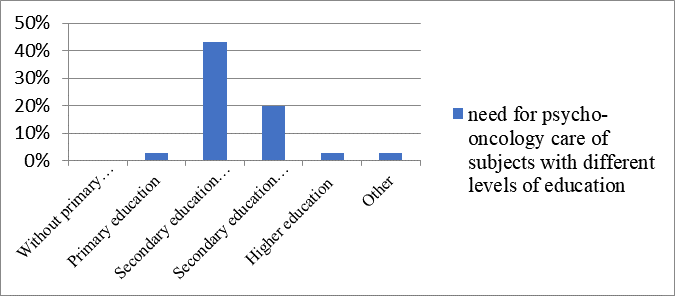
Regarding the education of subjects, in Chart 2 are the scores for psycho-oncological care of subjects depending on their level of education. From the results it can be noted that subjects without primary education, with primary and high education express less need for psycho-oncological care than subjects with secondary education. By subjects who have completed secondary education the need for psycho-oncological care is expresses at those who have completed general secondary education (gymnasium).
Family status is also taken as variable for analysis in this research and the results are presented in Chart 3. The data show that all subjects who have children and 77% of these subject need psycho-oncological care, where as 90% of subjects are married from whom 77% have need for psycho-oncological care.
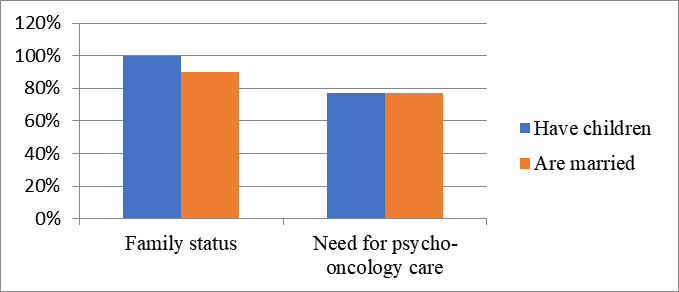
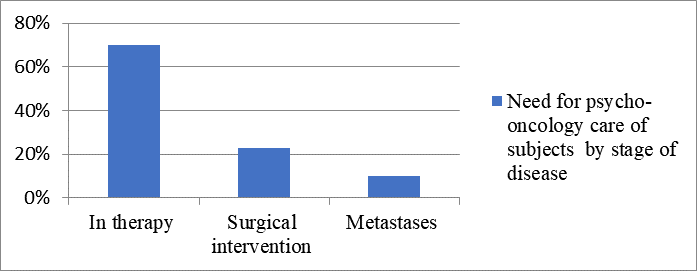
Percentage of the need for psycho-oncological care is analyzed also by the stage of disease development. The obtained data is for 3 categories of patients. Subject who are in therapy of which 70% have expressed a need for psycho-oncologycal care, where as the subjects who experienced an surgical intervention out of which 23% expressed such need and those who have metastases of which the need for psycho-oncological care is only 10%.
Conclusion
Psychological well-being has a significant impact on cancer suffering patients, who experience the disease and its consequences in different ways. Dealing with the illness is individual and always includes a major commitment.
The life of each patient was changed by changing his role in the family and lost his ability to work. Patients often count the family, their protection and security neglecting their health condition.
Fawzy (1999) describes five stages of illness experience: the first stage includes the findings of the diagnosis and provision of information which may cause the first effects of mental disorders; The second phase involves the treatment of disease, the stage where anxiety appear to therapy and its side effects; The third phase involves the break after the first treatment. At this time it creates space for depression, doubt, anxiety, but can also appear suicidal thoughts. Phase four is the progress stage of cancer and raises doubts; the fifth phase focuses on facing death, the inevitability and isolation (Fewzy, 1999).
The developement, manifestment of these phases also depend on the psycho-oncological care, psychological assistance from the staff, psychotherapy and social workers. A study showed that patients who are newly diagnosed, more than half of them have refused care by psychologists. This is described as a declining phase that includes protection mechanisms (Dorn, 2007).
In our study it was found that the subject aged 45-60 years old express more desire for psycho-oncological care (33%) than other groups involved in the research. Also subjects who have completed secondary school (43%) express a desire for psycho-oncological care more than subjects with other educational levels. These results can be gained by the disproportionate number of subjects in this categories, which also was one of the limitations of this research.
Regarding the treatment phase of the disease in this study we were not able to include newly diagnosed subject, so only subjects who are receiving therapy were involved, subjects who had an surgical intervention and subjectson metastasis. From these categories of subjects will for psycho-oncological care had subjects who are receiving therapy, meanwhile less willing subjects were those with metastases (10%). As well an indicator in this study is the family status. The results obtained for this indicator show that subjects who have children (77%) and are married in most cases express a desire for psycho-oncological care. Also we should note that pacients find the biggest support in coping with the disease and in the fight against the disease on their relatives, but important role in this process also play professionals who besides helping the patient, should help the other family members in the process of dealing and coping with the disease.
References
- Corbin, J.M., S.(1992). A. A nursing model for chronic illness management based upon the trajectory framework. in: P. Woog (Ed.) The chronic illness trajectory framework: The Corbin and Strauss nursing model. New York: Springer, 1992:9–28.
- Corbin JM, S. (1992). The Combin and Strauss nursing model.New York: Springer
- DGK, Deutsche Krebshilfe, AWMF. (2014). S3-Leitlinie Psychoonkologische Diagnostik, Beratung und Behandlung von erwachsenen Krebspatienten. Version 1.1 – Januar 2014 AWMF-Registernummer: 032/051OL
- Fewzy, I. (1999). Psychosocial interventions for patients with Cancer. European Jurnal of Cancer , 35.
- Jaspers, K. (1973). Allgemeine Psychopathologie. Berlin: Springer
- Keppling, J. (1998). Krebskrankheit und Partnerschaft.
- Keller, A. E. (1993). Hilfen bei der Mobilisierung persönlicher und sozialer Resoursen bei depressiven Krebspatienten. Stuttgart: New York.
- Krivo, B. (1998). Psycho-Oncologie. Holland: New York.
- Sahling, K. (2014). Erhaltung und Verbesserung der Lebensqualität bei einer Krebserkrankung. Berlin.
- Sun Min Lim, M.S., Hyeon Chang Kim, Gh. H., and Soohyeon Lee, S. (2013). Psychosocial Impact of Cancer Patients on Their Family Members.Cancer Research and Treatment: Official Journal of Korean Cancer Association.V.45(3) Sep. 2013; 226–233.
- Tschuschke. (2006). Psychoonkologie Psychologishe Aspekte der Entstehung und Bewältigung von Krebs. Stuttgart: Schattauer.
- Weis, J., Brocai, D., &Heckl, U. (2008). Psychoedukation mit Krebspatienten. Stuttgard: Schattauer
Copyright information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
About this article
Publication Date
20 May 2016
Article Doi
eBook ISBN
978-1-80296-008-2
Publisher
Future Academy
Volume
9
Print ISBN (optional)
-
Edition Number
1st Edition
Pages
1-104
Subjects
Psychology, clinical psychology, psychotherapy, abnormal psychology
Cite this article as:
Saliu, H. R., Rusi, M., & Kapllani, S. (2016). Need For Psycho-Oncologic Care On Pacients With Cancer. In Z. Bekirogullari, M. Y. Minas, & R. X. Thambusamy (Eds.), Clinical & Counselling Psychology - CPSYC 2016, vol 9. European Proceedings of Social and Behavioural Sciences (pp. 17-22). Future Academy. https://doi.org/10.15405/epsbs.2016.05.02.2

