Abstract
The outbreak of coronavirus disease in 2019-2020 has caused an intense disruption in the world as individuals and organizations recommend the significant factors in slowing down infection rates. One of the recommendations was keeping a social distance, which meant people would work from home, and some businesses would close down (
Keywords: Coronavirus diseaseCOVID-19digitalized healthcarehospital-at-homevirtual medical careonline healthcare
Introduction
Changes in the delivery of healthcare during the COVID-19 pandemic is inevitable since it is needed to mitigate staff exposure to infected persons, minimize the impact of patient surges at the health facilities and preserve personal protective equipment (PPE) (Bachireddy et al., 2020). Healthcare organizations have been forced to adjust the way they triage, care, or evaluate patients using methods that do not call for in-person services. One of the ways healthcare has adopted the use of online technological tools to continue offering healthcare from a distance and mitigate the virus (Rajasekaran, 2020). With the rapid development of information technologies and the increasing demand for medical services during the pandemic, healthcare was delivered through the Internet. The online health service (OHS) was provided to the people through various platforms such as websites, forums, and online communities. OHS is referred to as telehealth to incorporate communications that people have with their doctors through digital media such as computers and mobile devices. Most of these products and services were present before COVID-19, according to Hau et al. (2020). Still, many turned to use during the pandemic when they were restricted from visiting hospitals or making appointments with doctors due to the risk of transmitting the virus. This paper delves into the rate at which online health services were appreciated in the world map and widely used by most individuals due to the pandemic and the restraints instituted by the World Health Organization and the government.
Methodology
This study focuses on collecting credible information that best indicates the implications of online healthcare services during the COVID-19 pandemic. The study will employ the rapid literature review methodology to deliver evidence for this research. The quick review suggested in this paper is widely used by managers and clinicians who have limited time to find data they need in a timely fashion for making evidence-informed decisions. The review follows the six steps highlighted in the Figure
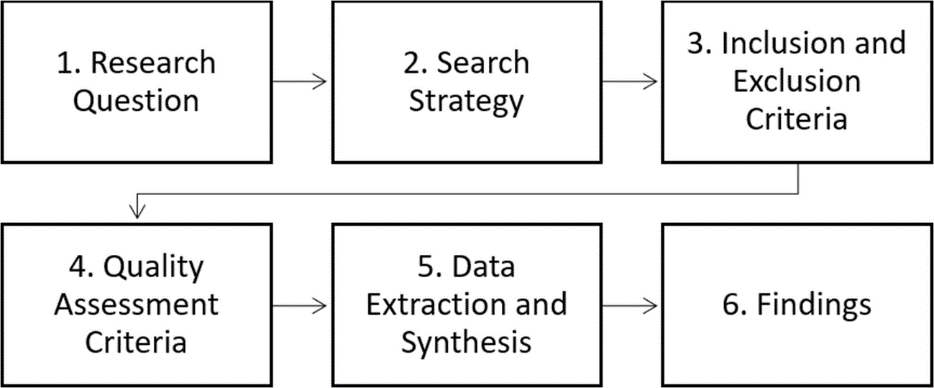
Research Questions
RQ1: What are the recommendations and challenges to telehealth, telemedicine, and cybernetic applications?
RQ2: What legislations are being followed to deploy online healthcare services during the COVID-19 contagion?
Search Strategy
The search strategy in this study will be employed to mark out relevant reviews with information that will be sufficient in answering the above research questions. The researcher formulated an online search of relevant peer-reviewed articles from the most renowned databases. Some of the databases utilized in the investigation include CORE, ScienceOpen, JSTOR, Cochrane Library, ERIC, MEDLINE, PsycINFO, PubMed, PubPsych, and Science Direct. The researcher will further consider information from government organizations such as the CDC and international bodies such as the WHO. Finding the relevant studies will be based on the keywords used, including telemedicine, online healthcare, telehealth, COVID-19, pandemic, coronavirus disease, remote care, digitalized healthcare, virtual healthcare, hospital-at-home, and virtual medical care. The search will consider the title and the year of publication, discipline, and publication category. The literature containing relevant information for this paper should be published within 1st May and 31st August 2020.
Recommendations and Challenges Towards the Use of Telehealth
Telehealth improves provider efficiency and productivity and improves their lives to encounter burnout. COVID-19 pandemic affected the familiar businesses with the world coming to a total shutdown. The significant recommendations pronounced by the government and the WHO included staying at home and avoiding social gatherings, washing hands with running water and soap, and wearing a mask at all times as established by Bryant et al. (2020). Most hospitals were overwhelmed with the numbers of COVID-19 cases, making it difficult for doctors to schedule regular appointments. Due to the fear of transmitting the virus, telehealth was further improved as its users tripled as indicated by Contreras et al. (2020); Louiselle et al. 2020). Most doctors would only schedule online appointments and meet their clients through various digital platforms such as clinical websites, Skype, and social media platforms. Some of the preferred websites include the likes of OrthoLive, initiated to offer clinical guidance and medical assistance to clients. OrthoLive would not only help to serve clients online but would also serve more clients since Orthopedics work in shifts and locum tenets.
Before launching a telehealth program during the pandemic, health organizations must ensure the systems are timely, safe, effective, efficient, equitable, and patient-centered. The services provided should be based on scientific knowledge to avoid non-beneficial services. The providers should deliver healthcare service that is respectful and responsive to individual preferences, values, and needs through the systems. Some of the earmarked challenges include interoperability and security in occasions where patients were expected to deliver information about their health or when the doctor seeks to relay test results to a client. With cybersecurity being a significant problem in healthcare operations, many users fear that the current systems can be hacked into and their data were stolen and manipulated (Maurrasse et al. 2020). Organizations that pride in their organizational culture have a hard time relaying the same while offering telehealth services. However, with advanced technologies, most of the systems allow and enhance team-based care by linking providers remotely for the sake of partnership and interchange of health data (Prasad et al., 2020). With the pandemic hitting hard and affecting almost all the countries across the world. Developing nations lack the necessary for full telehealth adoption because of the poor connection in some remote areas. The developing nations lack legislation to authorize telehealth implementation, hence making its focus during the pandemic difficult (Kadir, 2020).
Legislations Followed to Deploy Online Health Services
Telehealth is adopted to treat outpatient and triage to ensure minimal contact between the patient and the health practitioner with the ongoing pandemic. The US Department of Health and Human Services, together with the pharmacy board, are responsible for making legislations and reinforcing them. Amid a pandemic, these boards have temporarily altered their necessary requirements to accommodate telemedicine (Jaarsma et al., 2020). For instance, the medical personnel have been allowed to use non-HIPAA acquiescence digital tools including Skype, Zoom, FaceTime, and Cisco Webex to supplement the HIPAA compliant videoconferencing tools such as Updox, Microsoft Teams, Skype for Business, and VSee (Neubeck et al., 2020). Furthermore, the state pharmacy boards have temporarily allowed pharmacists to operate outside a licensed pharmacy because of the dangers of COVID-19. According to Hau et al. (2020), various institutions have drummed up support for telemedicine and telehealth, including the White House Coronavirus Task Force, which has directed medical stations to invest further in telehealth to enhance the quality of care across the country amid a global pandemic (Elson et al., 2020).
Discussion
The COVID-19 pandemic has vividly altered the average business in a health facility where outpatients receive healthcare. Telehealth is a measure taken by a healthcare organization to ensure its practitioners and outpatients' safety from transmitting coronavirus disease during face-to-face interactions (Goldschmidt, 2020; Pan, 2020). Telehealth has made it possible for the practitioner to conduct triage and necessary examinations and recommend the best drugs (Parisien et al., 2020). The pandemic has forced doctors to embrace virtual care because it was the only way to ensure that the population is safe from the virus and other illnesses (Hong et al. 2020; Meng et al., 2020). Telemedicine has been the doctor's first line of defense against coronavirus since it facilitates social distancing (Golinelli et al., 2020). The paper has established that telehealth has been widely applied globally in regions with good reception leaving out some of the low countries whose rural areas lack an excellent internet connection. This appears to be one of the demerits of using telehealth during the pandemic because it has successfully amplified socioeconomic inequalities. Some of the low individuals are discriminated against since telehealth requires mobile phones and the Internet, as cited by Elavarasan and Pugazhendhi (2020). It is imperative to establish that research conducted in 2019 indicated that only 4 billion persons worldwide have access to the Internet, with the usage disproportionally higher with the increasing income. However, Crawford and Serhal (2020) indicated that despite this challenge, telehealth is essential in educating patients and prompting a discussion with the physicians for further assistance. This study indicates that patients use telehealth to acquire health care from practitioners through the Internet in the midst of a pandemic.
Conclusion
In summary, online health services have existed for more than a decade, but 2020 marks the year the systems are more utilized globally due to the pandemic. The pandemic has made it possible for individuals to strike communications with professionals and colleagues through videoconferencing while working from home. Similarly, healthcare services have not halted but shifted from physical to online. Countries have compromised and relaxed some laws governing the health sector to facilitate healthcare through telehealth because of social isolation during the coronavirus. Some of the relaxed have allowed physicians to operate remotely while allowing medical doctors to diagnose their patients through videoconferencing. Some of the non-HIPAA compliant videoconferencing services have been allowed to serve the people with minimal restrictions. However, the growing use of telehealth among all people across the world makes it easy for hackers to hack into the hospital websites and forums to collect patient data. This is a significant challenge that could derail the application of telehealth across all parts of the world. The study has indicated that coronavirus has changed the way of life and allowed people to embrace technology more and value the modern ways of functioning.
References
- Bachireddy, C., Chen, C., & Dar, M. (2020). Securing the safety net and protecting public health during a pandemic: Medicaid's response to COVID-19. Jama.
- Bryant, M. S., Fedson, S. E., & Sharafkhaneh, A. (2020). Using Telehealth Cardiopulmonary Rehabilitation during the COVID-19 Pandemic. Journal of Medical Systems, 44, 1-2.
- Contreras, C. M., Metzger, G. A., Beane, J. D., Dedhia, P. H., Ejaz, A., & Pawlik, T. M. (2020). Telemedicine: Patient-Provider Clinical Engagement During the COVID-19 Pandemic and Beyond. Journal of Gastrointestinal Surgery, 1.
- Crawford, A., & Serhal, E. (2020). Digital Health Equity and COVID-19: The Innovation Curve Cannot Reinforce the Social Gradient of Health. Journal of Medical Internet Research, 22(6), e19361.
- Elavarasan, R. M., & Pugazhendhi, R. (2020). Restructured society and environment: A review of potential technological strategies to control the COVID-19 pandemic. Science of The Total Environment, 138858.
- Elson, E. C., Oermann, C., Duehlmeyer, S., & Bledsoe, S. (2020). Use of telemedicine to provide clinical pharmacy services during the SARS-CoV-2 pandemic. American Journal of Health-System Pharmacy: AJHP.
- Goldschmidt, K. (2020). The COVID-19 pandemic: Technology use to support the wellbeing of children. Journal of Pediatric Nursing.
- Golinelli, D., Boetto, E., Carullo, G., Landini, M. P., & Fantini, M. P. (2020). How the COVID-19 pandemic is favoring the adoption of digital technologies in healthcare: a rapid literature review. medRxiv.
- Hau, Y. S., Kim, J. K., Hur, J., & Chang, M. C. (2020). How about actively using telemedicine during the COVID-19 pandemic?. Journal of Medical Systems, 44, 1-2.
- Hong, Y. R., Lawrence, J., Williams, Jr. D., & Mainous Iii, A. (2020). Population-level interest and telehealth capacity of US hospitals in response to COVID-19: cross-sectional analysis of Google search and national hospital survey data. JMIR Public Health and Surveillance, 6(2), e18961.
- Jaarsma, T., van der Wal, M., Hinterbuchner, L., Köberich, S., Lie, I., & Strömberg, A. (2020). Flexibility and safety in times of coronavirus disease 2019 (COVID-19): Implications for nurses and allied professionals in cardiology.
- Kadir, M. A. (2020). Role of telemedicine in healthcare during COVID-19 pandemic in developing countries. Telehealth and Medicine Today.
- Louiselle, K., Elson, E. C., Oschman, A., & Duehlmeyer, S. (2020). Impact of COVID-19 pandemic on pharmacy learners and preceptors. American Journal of Health-System Pharmacy.
- Maurrasse, S. E., Rastatter, J. C., Hoff, S. R., Billings, K. R., & Valika, T. S. (2020). Telemedicine During the COVID-19 Pandemic: A Pediatric Otolaryngology Perspective. Otolaryngology–Head and Neck Surgery, 0194599820931827.
- Meng, X., Dai, Z., Hang, C., & Wang, Y. (2020). Smartphone-enabled wireless otoscope-assisted online telemedicine during the COVID-19 outbreak. American Journal of Otolaryngology.
- Neubeck, L., Hansen, T., Jaarsma, T., Klompstra, L., & Gallagher, R. (2020). Delivering healthcare remotely to cardiovascular patients during COVID-19: A rapid review of the evidence. European Journal of Cardiovascular Nursing, 1474515120924530.
- Pan, X. B. (2020). Application of personal-oriented digital technology in preventing transmission of COVID-19, China. Irish Journal of Medical Science (1971), 1-2.
- Parisien, R. L., Shin, M., Constant, M., Saltzman, B. M., Li, X., Levine, W. N., & Trofa, D. P. (2020). Telehealth utilization in response to the novel coronavirus (COVID-19) pandemic in orthopaedic surgery. The Journal of the American Academy of Orthopaedic Surgeons.
- Prasad, A., Brewster, R., Newman, J. G., & Rajasekaran, K. (2020). Optimizing your telemedicine visit during the COVID‐19 pandemic: Practice guidelines for patients with head and neck cancer. Head & Neck, 42(6), 1317-1321.
- Rajasekaran, K. (2020). Access to Telemedicine—Are We Doing All That We Can during the COVID-19 Pandemic? Otolaryngology–Head and Neck Surgery, 0194599820925049.
Copyright information

This work is licensed under a Creative Commons Attribution-NonCommercial-NoDerivatives 4.0 International License.
About this article
Publication Date
09 October 2022
Article Doi
eBook ISBN
978-1-80296-949-8
Publisher
European Publisher
Volume
1
Print ISBN (optional)
-
Edition Number
1st Edition
Pages
1-95
Subjects
Health psychology, psychology, health systems, health services, social issues, teenager, children's health, teenager health
Cite this article as:
Jaworski, M. (2022). Implications Of Online Health Services During Covid-19. In M. Jaworski (Ed.), Health & Health Psychology - icH&Hpsy 2020, vol 1. European Proceedings of Health (pp. 1-6). European Publisher. https://doi.org/10.15405/eph.20101.1

